The RECAP preterm Cohort Platform
Here you can access the heart of RECAP preterm: our cohort platform. At the moment, there are 27 individual studies, 101 collected datasets and 13,716 individual study variables available.
If you would like to have more information, please get in contact!
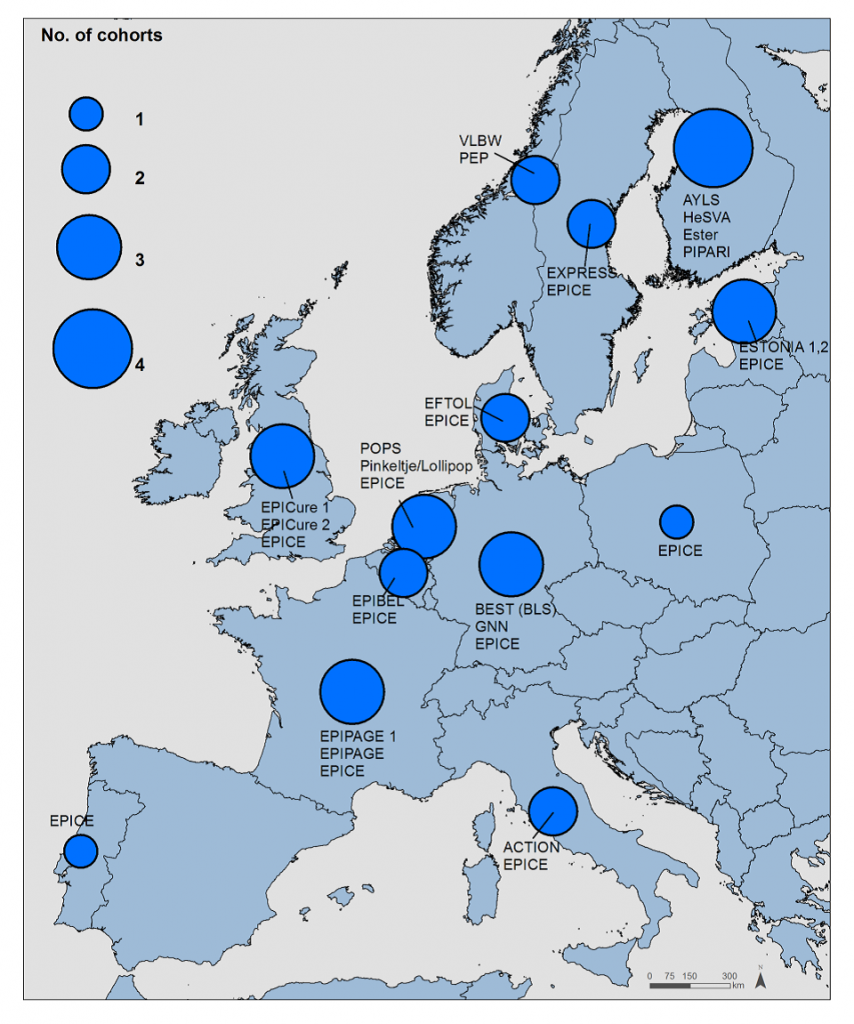
The RECAP preterm Cohort Platform brought together 20 population-based cohorts with children born very preterm or with very low birth weight (VPT/VLBW cohorts) from 13 European countries as well as the multiple stakeholders who have been involved in their development and use: Obstetricians, neonatologists, pediatricians, psychologists, psychiatrists, other health care providers, educators, basic scientists, economists, policy planners, health insurance companies and patient and parent groups.
The data from the cohorts is further enhanced by pooling whole-country registry linkage studies from four Nordic countries. Pooled data from the combined cohorts, together with the registries, allow for high-powered analyses of less common health outcomes and of the effect of specific risk and universal or specific resiliency factors.
The existing very preterm birth cohorts contain prospectively followed populations of particularly vulnerable children of different age ranges from a number of countries over a wide historical time span. They include exposures to variable and contrasting health care and technological interventions available at different points in time. The historical time span and geographical diversity of the cohorts provided a unique opportunity to generate evidence that have greater generalizability than the cohorts individually.
Thanks to the RECAP preterm Cohort Platform our project did:
Make major conceptual, methodological and analytical contributions towards integrated cohorts of VPT/VLBW born across Europe and beyond and allows for their efficient exploitation.
Our cohorts were integrated by constructing a harmonized data platform that combines cohort data for VPT/VLBW in Europe and beyond. Efficient exploitation was ensured by giving stakeholders such as scientists, clinicians and parents free access to the platform which enables them to find answers to their questions and needs.
A major conceptual contribution towards integration is to harmonize the data into the platform in a way that exploits the strengths of each separate cohort. Our major innovative methodological contribution consists of combining data from VPT/VLBW cohorts, and in addition, with health registry data from the Nordic countries. A major analytical contribution was made by implementing an innovative new three-step data harmonization process using novel statistical methods.
The platform combined and harmonized data from all European VPT/VLBW-cohorts illustrated in the overview map. In addition, collaboration from the APIC consortium (Australia, New Zealand, Canada, USA) resulted in a world wide data base that is further sustainable after the project completion.
Contribute to providing novel information on health maintenance, onset and course of diseases in the area of physical and mental health and use population stratification to better tailor diagnosis or to optimize prevention and treatment.
Risk research only tells the story for those persons who develop disease after exposure. However, much can be learned for optimization of prevention and treatment from those who beat the odds and develop adaptively and disease free after risk exposure – a positive deviance approach.
The research in the demonstration projects (WP 6 – 9) generated new information on health maintenance, onset and course of disease and overall social and economic adaptation from birth to adulthood. The bringing together of cohorts and registry studies allowed us to determine the impact of events that are rare in the general newborn population but frequent in VPT/VLBW populations. It allowed us to determine universal (replicated across cohorts and settings) and specific risk factors in context. The combined database allowed for population stratification not usually possible in single cohorts.
A life course longitudinal approach allowed us to determine protective and resiliency factors after VPT/VLBW birth. The identification of universal factors helps clinicians, educators, health providers and policy makers across Europe to provide more accurate prognoses for patients and initiate appropriate remedial or anticipatory actions. This was done by developing a prognostic scoring system taking into account pre- and neonatal complications, early functional developmental follow-up indicators and social context. There are also be country-specific protective factors that help to inform how changes in treatment could be beneficial in other contexts.
Go beyond considering disease and social adversities in silos but provide information on their combined impact on the social and economic and quality of life consequences of being born VPT/VLBW and inform general or specific support services.
Particularly novel is the interdisciplinary approach and the richness of the data. Health maintenance and onset and course of disease, whether physical or mental, is usually multifactorial and strongly dependent on social and environmental influences after the initial exposure. The longitudinal studies went beyond uni-factorial approaches only looking at risk to outcomes relationships. Instead, these studies were able to determine developmental trajectories and changes over time influenced by both social and post-discharge treatment factors. This helped determine groups of individuals who are at increased probability to develop disease or adverse outcomes within defined environmental contexts. This allows for much improved prognosis of long term outcomes.
Furthermore, the consequences of VPT/VLBW on life chances (economic, building friendships and finding a romantic partner) and the quality of life and life satisfaction are major outcomes that are becoming more and more important in assessing the value and cost-effectiveness of interventions. RECAP preterm was able to determine across the life course the influences of medical treatment, childhood experiences, psychosocial and educational interventions on economic and social adaptation as well as quality of life and life satisfaction. Understanding whether there are specific factors for VPT/VLBW who improve their lives or universal factors (e.g. good relationships to peers, parents) that increase their quality of life are highly important for planning support services for VPT/VLBW survivors.
Provide the evidence base for the development of policy strategies for prevention, early diagnosis, therapies, health economics as well as addressing health inequalities.
The integration of analysis across cohorts and several registry studies does not only lead to increased statistical power to analyze multiple risks and exposures but also helps identify protective and resiliency factors. This provides invaluable information on how and when to intervene, where to focus preventive measures and what early diagnoses are valuable to predict long term outcome.
Moreover, it is possible to evaluate which early diagnoses and therapies after hospital discharge have been effective (e.g. occupational and physiotherapy, psychological therapies, educational support, language therapy etc.), i.e. lead to altered trajectories of outcome in various areas (motor, health, mental health, service use etc.). Most importantly, cohort and registry studies have detailed data on schooling, usually the largest cost related to VPT/VLBW birth. For example, special schooling is three or more times more expensive than regular schooling and additional help at home and within school for those in regular school adds to costs.
The wealth of data on socio-economic and family factors provided a comprehensive picture on health inequalities that may impact VPT/VLBW particularly. Beyond usual indicators, consequences on parent employment and careers, outcomes of siblings of VPT/VLBW children, extra costs for care and effects on the individual such as fertility were estimated. RECAP preterm provided a much more complete picture of the consequences and influential factors leading to adverse (and adaptive) outcome with important implications for strategies for prevention.
Evaluate the economic outcomes associated with VPT/VLBW, including health utilities and economic costs to health systems such as targeted aftercare planning to improve quality of life, costs to other sectors of the economy and costs for individuals and families.
Many of the older child cohorts and all the adult cohorts include measures of quality of life and health utilities. Apart from documenting whether quality of life increases or decreases from childhood into adulthood, it was possible to investigate what areas of child and adult functioning (VPT/VLBW birth, physical disability, mental health, social relationships etc.) are associated with impaired quality of life and what changes in these parameters are related to decrements or increments in health utility. This identified areas that are of most relevance to the quality of life of affected VPT/VLBW individuals and their parents and provide crucial information where resources should be targeted to improve their health outcomes. It had direct consequences for policy and after care planning.
Lead to the optimization of the use of population cohorts in defining/improving clinical practice and public health policy.
The value of a new innovative data resource depends not only on the quality of the data, their harmonization and accessibility but also on the use that is made by different stakeholders.
We therefore would like to see our data platform being used well beyond the RECAP preterm Project by researchers from different disciplines interested in the outcomes of VPT/VLBW in disease processes. To facilitate this we worked closely with a range of stakeholders, ranging from neonatologists to those working with VPT/VLBW children (teachers, social workers) to policy makers, to make sure the platform meets stakeholder needs, which is essential in improving clinical practice and public health policy.
Have a major infrastructure effect by enabling researchers and clinicians across Europe and worldwide to conduct VPT/VLBW cohort research at reduced cost and at better value for money.
The innovative data resource with its interfaces and partly automated harmonization algorithms enables researchers and clinicians around Europe and also transitional countries to use the resource as a platform in future applications for cohort research on VPT/VLBW populations. It enhances their chances of funding using an established platform for data management and create better value from investments by funders. It also serves as a model for developing similar resources for population cohorts outside the field of VPT/VLBW research.
